Circadian rhythms sleep disorder
Sleep, as well as other functions of the organism (hormones, metabolism, etc.) is regulated by the “biological clock”. This is a neuronal center in the hypothalamus of the brain which is responsible for signaling to the rest of the structures of the brain to initiate and end sleep. In this way, it is the biological clock that sets the time at which the propensity for sleep increases and decreases. When activated, the biological clock sends a signal to the pineal gland, located next to the brain, to begin the production of melatonin. This hormone coordinates the adjustment of the remaining functions of the organism to start the period of sleep.

Learn more about this pathology

Under normal conditions, the biological clock is synchronized with the external brightness and receives information directly through the retina. Thus, in natural conditions, the biological clock is activated at the end of the day by the decreasing light signal, so we notice the feeling of sleepiness a few hours later. However, exposure to the artificial light of the modern world and, more recently, night exposure to televisions, computers, tablets, etc. may cause the brain centers that regulate sleep not to be activated until several hours later.
Under normal conditions, sleep regulating centers receive the activation signal in the evening, and this makes us feel sleepy at that time. They are progressively disabled in the morning. However, the biological clock can be altered for several reasons, such as:
- Genetic factors: several genes (collectively called “clock genes”) are involved in this process and any genetic abnormality in them may make it difficult to sleep at certain times.
- Hormonal factors: different hormonal changes which occur during menstruation, menopause, but also in some endocrine diseases, can alter the function of the biological clock.
- FMedications: some drugs with effects on the nervous system, such as antidepressants, but also some antihypertensives, alter the sleep-wake rhythm.
- Ophthalmologic disorders that hinder the transmission of the light signal.
- Neurological disorders
- Age.
- Diet, exercise, etc.
All of these situations can lead to an inability to sleep at the beginning of the night, problems or difficulties staying asleep in the morning, or staying awake during the day.
How do I know if my insomnia problem is due to the brain clock malfunctioning?
It is always important to keep in mind that insomnia may frequently be due to abnormal functioning of the biological clock, rather than inadequate relaxation or poor stress management.
How do I know if circadian rhythms are involved in my insomnia?
If you can sleep well, although not at the time you want or think that you should sleep, it is possible you suffer from a disorder of sleep rhythm. For example, some people sleep well between 6am and 2pm, or between 7pm and 2am in the morning, but cannot sleep when they seek to do so between 11pm and 7am in the morning. In some rare cases, insomnia occurs in a periodic manner, i.e., during every period of five weeks they have insomnia for two weeks.
Some specific indicators that a problem with insomnia may be mainly due to a dysfunction of the sleep-wake rhythm are:
- Difficulty falling asleep, mainly when trying at the beginning of the night (to a much lesser degree if trying at other times) or
- Difficulty staying asleep, mainly when trying at the beginning of the night (to a much lesser degree if trying at other times).
- The problem began in adolescence or even in childhood.
- The problem occurs almost daily, regardless of stress levels or the environment in which one sleeps.
- Aggravation of the problem when crossing several time zones (depends on the type of problem and the direction in which we travel).
- Improvement in the insomnia with administration of melatonin.
- The night insomnia problem is associated with hypersomnolence during the day, i.e., no difficulty sleeping at certain times of the day.
- Family affected by a similar problem.
Some types of insomnia caused by alteration of the sleep-wake rhythm:
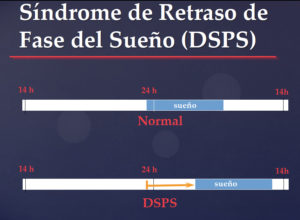
DELAYED SLEEP PHASE SYNDROME
Some people have difficulty sleeping at regular hours (e.g., at 11 or 12 at night). At that time they are wide awake and, even when they know they have to get up early the next day, they are unable to fall asleep. They only fall asleep hours later, usually when it’s already early morning. Once they fall asleep, they sleep deeply, not waking up in the night beyond what is normal for their age. If they have to get up early, it is very hard for them to get up, if they have fallen asleep. In such cases, they go about their activities despite having slept few hours, feeling tired, sleepy, and performing inefficiently during the morning. Throughout the day their discomfort decreases and they feel relatively well at night. Due to the insufficient number of hours they sleep during the week, they tend to compensate for the lack of sleep on the weekends, falling asleep in the early morning and waking up at noon, and at times, in the afternoon. During the holidays, now free of working hours, they rise late in the morning, and by sleeping a sufficient number of hours, their symptoms of sleepiness and discomfort disappear.
In short, what is characteristic of these people is that their sleep is normal in quantity and duration but takes place at a late hour. It is called delayed sleep phase syndrome. In some people it occurs with greater severity, for example, falling asleep at 4 or 5 in the morning, but in many others it may manifest in a more mild way, for example, struggling to fall asleep before 1 in the morning and just sleeping 1 or 1.5 hours less than they should.
ADVANCE SLEEP PHASE SYNDROME
This is the opposite situation: the sleep cycle begins early (e.g. at 8pm), and also ends early (in the early morning). The affected people often feel at most a certain tiredness in the evening, which turns into drowsiness if they perform sedentary tasks (e.g. driving). Once in bed, they usually fall asleep quickly. However, at midnight they wake up wide awake, and this is their main complaint.
This situation is more common in older people, contrary to delay syndrome which is more common in the young. It may also occur in certain families, and there is a gene associated with this condition.

IRREGULAR SLEEP RHYTHM
This occurs when there is a full fragmentation of the sleep rhythm, such that it occurs randomly in episodes never exceeding several hours both at night and during the day. It mainly occurs with some neurological disorders. However, in its minor form, all psychophysiological insomnias end up having some amount of irregularity in the sleep rhythm.

JET-LAG
Jet lag occurs when we expose a person to a sudden change of schedule, with usually three or more hours of difference. Since the change occurs abruptly, the internal biological rhythm of sleep is outdated with respect to the new local time. Between the US and Europe there are six or more hours of time difference. Therefore, travelers who take a plane from Boston at 7pm (local time), land in Madrid at 9am (local time). At that time their biological clock is still at 3 am and, more importantly, their body is working as if it was still 3 am. This is the main reason why they feel tired and intellectually impaired upon arriving at the new destination.
Their mind runs slowly, with very little clarity. They are irritable, their reactions occur slowly, and they suffer from gastrointestinal upset. Upon arrival to their destination, their body will need several days to adapt gradually to the new schedule. The speed of adaptation will depend on several factors, which include the time difference between the starting point and the destination, the patient’s age, exposure to ambient light, etc.
Throughout the first day, travelers will notice that they are already sleepy at mid-afternoon and that during the first night suffer from frequent awakenings and are wide awake early in the morning. Their sleep is not restorative. Over the following days, the tendency to fall asleep and wake up early will decrease, probably at a rate of 1.5 hours per day that has elapsed.
Young people tend to have greater problems when flying from the west towards the east (Boston to Madrid), since they have a longer sleep cycle that must be compressed into a shorter day. The opposite occurs in the elderly: for them it is more difficult to travel east to west (Madrid to Boston) because they have a short sleep cycle and must adapt to an especially long day.
Jet lag does not depend on the duration of the trip, but only on the number of time zones crossed. Thus, there is no Jet Lag when flying from Scandinavia to South Africa. Not everything that we call jet lag is actually jet lag. Traveling from west to east (e.g., America to Europe), during the first day, in addition to jet lag, we are experiencing a suppression of sleep (in fact we wake up early in the morning!). Moreover, it is likely that during the days prior to the trip, we have slept less than usual. On the other hand, the effect of sitting on the plane for so many hours, not being able to sleep (noise and discomfort), changes in eating, stress associated with travel, or the effect of a closed environment or smoking areas favor a situation of exhaustion and fatigue. Whatever it is, all of these factors contribute to the same result as jet lag: fatigue. The schedule lag also prevents quick recovery at the destination since adaptation occurs slowly.