Sleep Apnea Syndrome
There are people who, in addition to snoring, suffer repeated pauses in breathing that vary in length. Pauses lasting more than 10 seconds are more clinically important. These can sometimes reach 60 or 120 seconds. It is characteristic of apnea for these breaks to be interspersed between snoring.
The emergence of sleep apnea is due to a total collapse or almost total (in the case of hypopneas) collapse of the interior of the pharynx. Apneas entail a transient cessation of breathing and should not be confused with cardiorespiratory arrest, since during apneas the heart continues to beat. Upon stopping breathing, there is a transient drop in blood oxygen levels . If the apneas are very frequent, the affected person will continue to have low blood oxygen levels for a good part of the night.
Learn more about this pathology
One of the most significant consequences of sleep apnea is the fragmentation of sleep: whenever an apnea occurs, it ends with an arousal of a few seconds, less than the time required to remember it in the morning. The succession of these microarousals (at least as many as there apneic episodes) causes the person who suffers from them wake up feeling unrested, even though they may not recall being awakened during the night. However, in these individuals a headache is usual upon waking (which improves within a few hours), as well as a dry mouth. In addition, apnea causes daytime tiredness and sleepiness in sedentary situations. It is characteristic to have an increased risk of traffic accidents (up to seven times higher than the normal population) and work-related accidents. Changes in mood, such as irritability and depression, changes in performance, memory, or loss of the ability to concentrate have also been reported.
In cases of severe apnea, aside from the aforementioned problems, there is an increased risk of diseases such as high blood pressure (more than 40% of patients with apnea suffer from hypertension), increased risk of ischemic heart disease (chest pain, and even heart attacks) and stroke. Failure to follow treatment can lead to an increase in mortality figures over the years.
The risk of this disorder increases with age, reaching a peak between the fifth and seventh decades of life. Predisposing factors are the same as for snoring and nearly all those who suffer from sleep apnea are more or less significantly overweight. It is, on the other hand, a typically male disease, with an incidence 2.5 times higher in men than in women, although the incidence in women increases starting at menopause.
The essential test to diagnose sleep apnea is a sleep study, with polysomnography being the most accurate and providing the most information. It requires spending a night in a sleep center. While it is possible that sleeping in a sleep center may affects sleep, it still allows clinicians to examine how a patient breathes while sleeping. Measurements are taken of the respiratory flow, the effort that is made to breathe, the level of oxygenation of the blood, the functioning of the heart and the quality of sleep. Without this test, it is impossible to exclude the possibility of sleep apnea.
TREATMENT OF SLEEP APNEA
- With respect to the actions that needs to be taken for sleep apnea, general prevention measures must be taken in all cases, similar to those actions recommended to prevent snoring, but given the greater severity of apnea, they should be carried out with greater commitment. Briefly these are: weight loss, (to make weight loss more effective, it is usually helpful to be followedby a nutritionist); avoiding sleeping on the back; avoid drinking alcohol, using tranquilizers or tobacco; exercise moderately in the evening.
- There can be several types of surgical options, but all are based on an examination by a specialist in otolaryngology, during which the structure of the airways are examined in detail. The type of operation depends on the location and the significance of the abnormalities found: if there is an abnormality in the nasal passages, a correction of the nasal septum or a resection of polyps, etc. can be done. A resection of the soft palate is more common (this is an operation generally called UPPP or uvulopharyngopalatoplasty). Sometimes several techniques are combined or are performed in a serial fashion over time. The percentage of patients who permanently resolve their issue is about 30-50% and there is no guarantee an individual will be cured. In general, the odds of success are greater in non-obese patients with a clear anatomical abnormality and in those who do not have severe apnea before the operation.
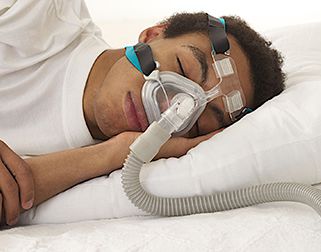
- The treatment of choice, at least for the most severe cases, is treatment with positive airway pressure (more commonly referred to by its initials, CPAP). It consists of a nasal or nasal-mouth mask, used at night every time one goes to sleep. It is connected by a tube to a small device that is placed on the bedside table. The CPAP device is an air compressor, which emits a current of air that is breathed in and prevents the airway from collapsing, allowing normal breathing throughout the night. The percentage of patients who solve their problem using the CPAP is very high (above 90%). Within the first days of treatment there is usually a clear improvement in daytime sleepiness, as well as a great sense of well-being upon waking. Nonetheless, it should be noted that CPAP treatment is not curative and is only useful for the duration of its use. In some cases, it is used while the patient tries to lose weight.
- In short, there are different types of treatment for sleep apnea. The selection of the most appropriate one must be chosen individually and according to a plan that should be made in conjunction with a specialist.